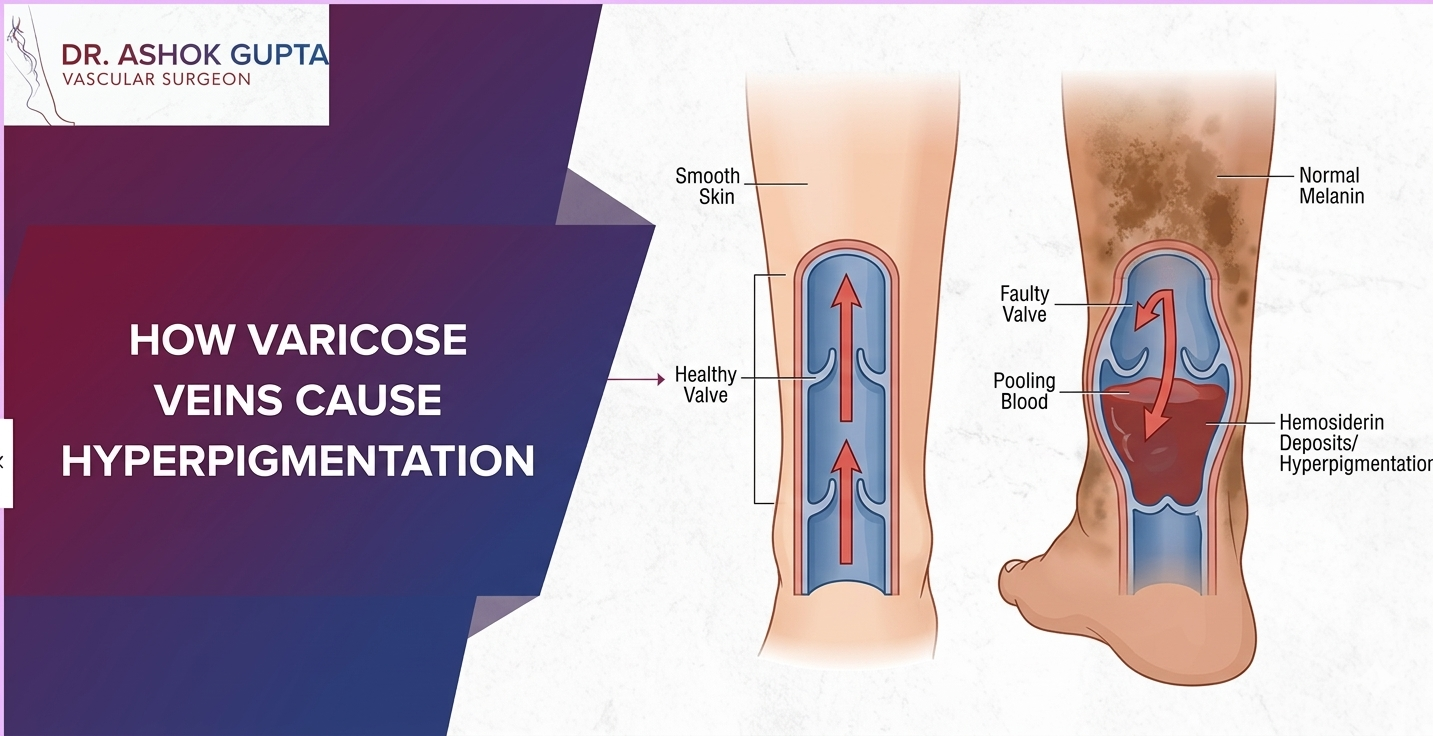
Stasis Dermatitis: Why Skin Health Depends on Vein Health
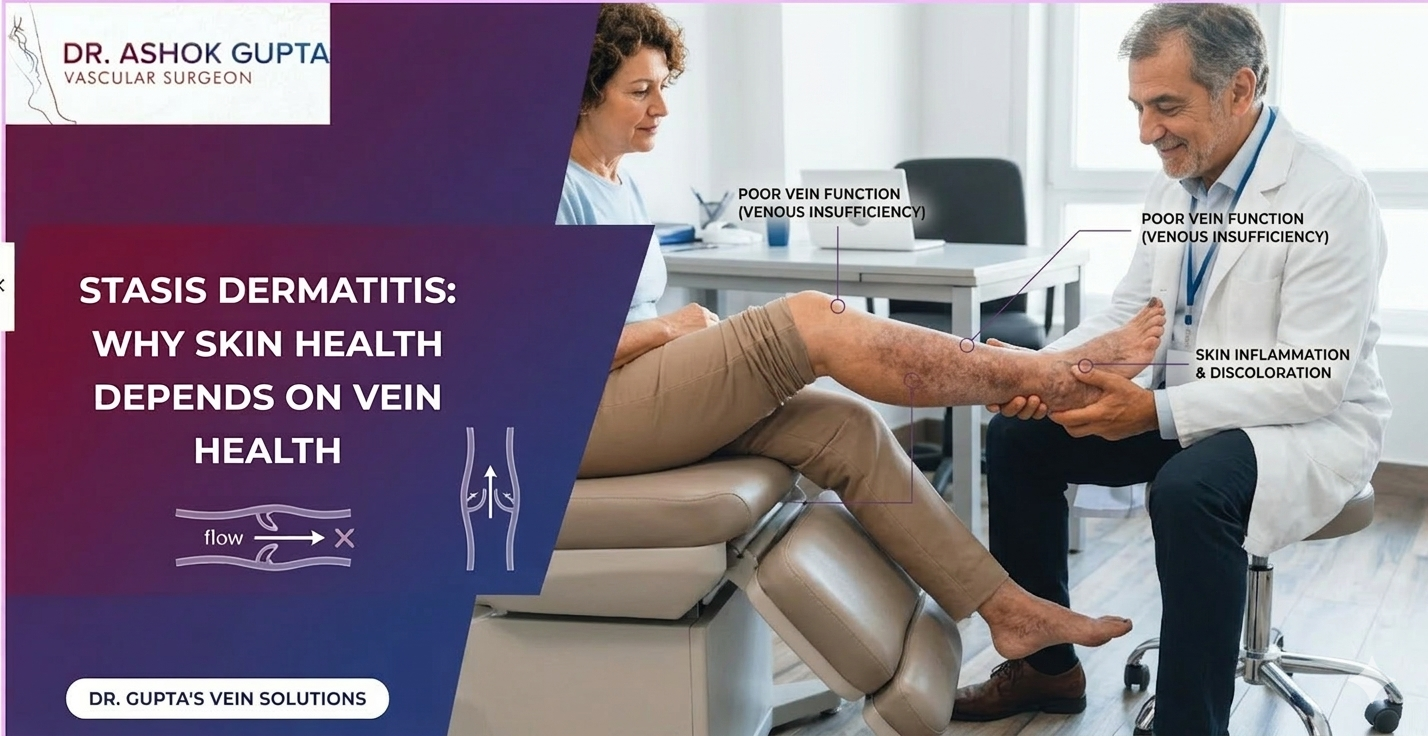
Pulmonary embolism is one of those diagnoses that can sound distant until it happens to someone close. In many cases, it starts quietly as a blood clot in the leg, then turns dangerous when the clot breaks apart and moves to the lungs. From a vascular surgeon’s point of view, the most important message is that a pulmonary embolism is a medical emergency. Still, it is also highly treatable when it is recognised early.
This article explains what is a pulmonary embolism, where blood clots form in the leg, the warning signs people miss, and what modern pulmonary embolism treatment looks like.
Healthy Veins, Happier Skin!
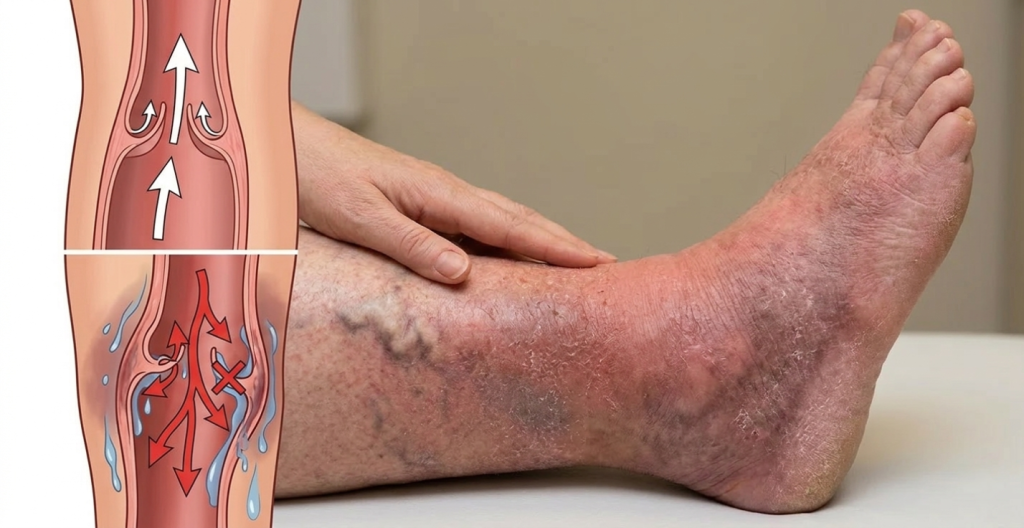
Have you noticed persistent redness, itching, or darkening on your lower legs? Does the skin around your ankles look dry, irritated, or swollen?
Many people ignore these signs, thinking it is just “dry skin” or a rash. But sometimes, your skin is trying to tell you something important about your veins.
One common but often misunderstood condition is Stasis Dermatitis. It is a skin problem linked closely to poor vein function. The good news? With the right care and timely treatment, it can be managed well.
Let’s understand this step by step, in a simple and practical way.
What is Stasis Dermatitis?
Stasis Dermatitis is a type of skin inflammation that happens when blood does not flow properly in the veins, usually in the legs. Doctors also call it venous stasis dermatitis.
Your leg veins have a big job. They must push blood back to the heart against gravity. Tiny valves inside the veins help with this. When these valves become weak or damaged, blood can pool in the lower legs. This is called venous insufficiency.
When blood pools, pressure builds up. Fluid and blood cells can leak into nearby tissues. Over time, this irritates the skin. That irritation shows up as stasis dermatitis.
So, in simple words: Unhealthy veins can lead to unhealthy skin!
Why skin health depends on vein health?
Your skin needs good blood flow to stay healthy. It needs oxygen and nutrients. It also needs waste products to be cleared away.
When veins do not work well:
- Blood collects in the lower legs
- Pressure rises in the veins
- Fluid leaks into the skin
- Inflammation begins
This creates redness, itching, swelling, and skin damage. If ignored, it can even lead to sores called venous ulcers.
So, treating only the skin is not enough. The root cause often lies in the veins.
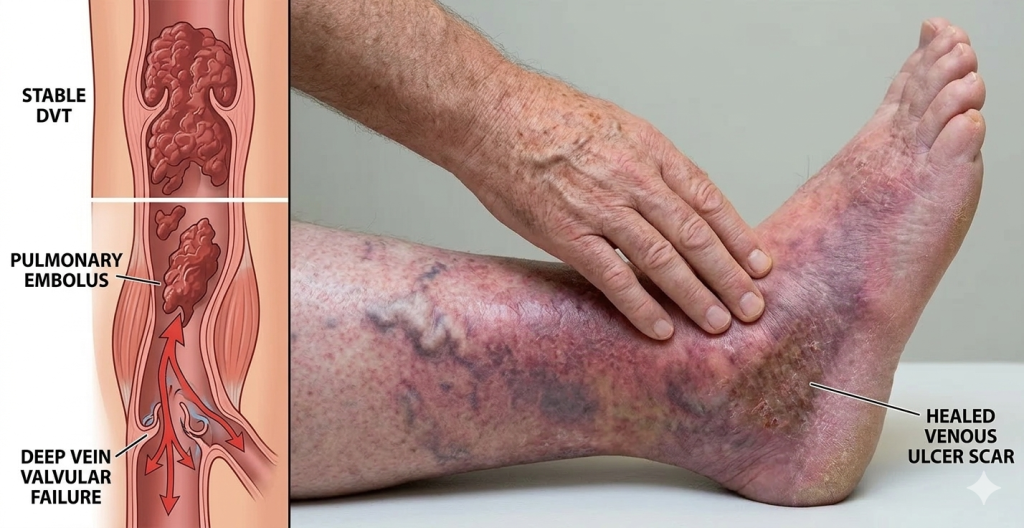
What are the causes of Stasis Dermatitis?
Some of the most common stasis dermatitis causes include:
1. Chronic venous insufficiency
This is the main cause. The veins struggle to return blood to the heart.
2. Varicose Veins
Twisted, enlarged veins often mean the valves are weak.
3. Previous DVT (Deep Vein Thrombosis)
A past clot can damage vein valves.
4. Long periods of sitting or standing
This slows down blood flow in the legs.
5. Obesity
Extra weight puts more pressure on leg veins. The more risk factors you have, the higher the chance of developing stasis dermatitis.
Stasis Dermatitis stages
Stasis dermatitis usually develops gradually. Knowing the stages helps you seek help early.
Stage 1: Early changes
- Mild swelling in ankles
- Skin feels itchy or dry
- Slight redness
Many people ignore this stage.
Stage 2: Visible skin changes
- Red or brown discoloration
- Thickened or scaly skin
- Persistent itching
- Tenderness
At this point, skin damage is clearer.
Stage 3: Advanced stage
- Dark patches on the skin
- Hard or leathery skin
- Oozing or crusting
- Pain or burning
Stage 4: Complications
- Open sores (venous ulcers)
- Risk of infection
- Slow wound healing
Early treatment can prevent reaching later stages.
What are the symptoms to watch for?
See how many of these you notice:
- Itchy lower legs
- Swollen ankles
- Red or brown skin near ankles
- Dry, flaky skin
- Aching or heavy legs
- Skin that feels warm or tight
If you checked several of these, it is wise to see a vascular specialist.
What are the treatment options for Stasis Dermatitis?
Here is the encouraging part: Stasis Dermatitis treatment is possible and effective, especially when started early.
Treatment focuses on two things:
- Improving vein function
- Healing and protecting the skin
1. Compression therapy
Compression stockings help blood move upward. They reduce swelling and pressure. This is often a key part of treatment.
2. Leg elevation
Raising your legs above heart level helps blood flow back. Try this a few times a day for 15–30 minutes.
3. Medical treatment for veins
Dr. Ashok Gupta may recommend:
- Minimally invasive vein procedures
- Treatment for varicose veins
- Management of venous insufficiency
Treating the vein problem helps prevent recurrence.
4. Skin care
Gentle skincare is essential.
- Use mild cleansers
- Moisturize regularly
- Avoid scratching
5. Medications
Doctors may prescribe creams or medicines to reduce inflammation or infection.
Surgical Treatment Options
Here are some commonly used options:
1. Endovenous Laser Treatment (EVLT)
This is a modern and widely used procedure.
- A thin laser fiber is inserted into the faulty vein
- Laser energy gently heats and seals the vein
- Blood naturally reroutes to healthier veins
It is done under local anesthesia. Recovery is usually quick. Many patients walk the same day.
2. Radiofrequency Ablation (RFA)
This is similar to laser treatment but uses radiofrequency energy.
- A catheter delivers controlled heat to the vein wall
- The vein closes and stops pooling blood
RFA is known for minimal discomfort and fast recovery.
Sclerotherapy
Sclerotherapy works well for smaller varicose veins.
- A special solution is injected into the vein
- The vein collapses and fades over time
Multiple sessions may be needed in some cases.
Microphlebectomy
This is used for visible varicose veins near the skin surface.
- Tiny incisions are made
- The damaged veins are gently removed
Scars are very small and often barely noticeable.
Venous Ulcer procedures
If stasis dermatitis has led to ulcers, treatment may include:
- Advanced wound care
- Debridement (removal of unhealthy tissue)
- Skin grafting in selected cases
These help wounds heal faster and reduce infection risk.
Usage of VenaSeal (Bio-Glue) for Stasis Dermatitis by Dr. Ashok Gupta
For many patients with Stasis Dermatitis, the real problem lies deeper than the skin, in the unhealthy veins beneath. When creams and compression give only temporary relief, treating the faulty vein becomes important. This is where VenaSeal (bio-glue therapy) can play a valuable role.
Dr. Ashok Gupta offers VenaSeal as an advanced, patient-friendly option for suitable cases of venous insufficiency linked to stasis dermatitis.
What is VenaSeal?
VenaSeal is a minimally invasive vein treatment that uses a specially formulated medical adhesive (often called “bio-glue”) to close damaged veins.
Instead of heat or laser energy, this method seals the vein using adhesive. Once the vein is closed, blood automatically shifts to healthy veins. This reduces blood pooling, pressure, and inflammation in the legs, key triggers behind stasis dermatitis.
How VenaSeal helps Stasis Dermatitis?
By sealing the faulty vein, VenaSeal helps:
- Reduce venous pressure
- Decrease leg swelling
- Improve skin nutrition
- Lower inflammation
- Support healing of irritated skin
- Reduce risk of ulcers
As circulation improves, the skin often becomes less itchy, less swollen, and healthier in appearance.
What is the best cream for Stasis Dermatitis?
Many patients ask this. The honest answer is:
The best cream depends on your condition.
Doctors often recommend:
- Medicated steroid creams to reduce inflammation
- Moisturizing creams to repair the skin barrier
- Antibiotic creams if infection is present
However, self-treatment is risky. Some creams can worsen the problem if used wrongly. Always consult a specialist before using medicated creams.
Can lifestyle changes help?
Absolutely. Small steps make a big difference.
Try these:
- Walk regularly to improve circulation
- Avoid sitting or standing too long
- Maintain a healthy weight
- Elevate legs when resting
- Wear compression stockings if advised
- Remember, consistency matters more than perfection.
When should you see a specialist?
Do not wait if you have:
- Persistent leg swelling
- Skin color changes
- Ongoing itching or rashes
- Open sores on the legs
- Painful varicose veins
Early care prevents complications.
How Dr. Ashok Gupta can help you?
Dr. Ashok Gupta focuses on identifying the root cause behind vein-related skin problems. His approach is patient-friendly and practical.
He may use:
- Detailed vein evaluation
- Ultrasound scans
- Customized treatment plans
- Minimally invasive vein care
The goal is not just symptom relief, but long-term vein health.
Experience improved vascular health. Get in touch with Dr. Ashok Gupta today.
FAQs
What is the main cause of stasis dermatitis?
The main cause is poor blood flow in the leg veins, called venous insufficiency. When veins cannot push blood back to the heart properly, blood pools in the legs and irritates the skin.
How do you get rid of stasis dermatitis?
It improves by treating the vein problem and caring for the skin. This may include compression stockings, leg elevation, proper skincare, and medical or minimally invasive vein treatments.
What does stasis dermatitis look like?
It often appears as red, itchy, dry, or scaly skin on the lower legs or ankles. Over time, the skin may turn brownish, thick, or swollen.
What is the best medication for stasis dermatitis?
There is no single “best” medication for everyone. A doctor may use steroid creams for inflammation, moisturizers for dryness, or antibiotics if infection is present. The right choice depends on your condition.